ACL Reconstruction Technique
Comprehensive guide to ACL reconstruction surgical technique for FRCS exam preparation
Reviewed by OrthoVellum Editorial Team
Editorial maintenance, source checking, and correction workflow • Published by OrthoVellum Medical Education Team
ACL RECONSTRUCTION TECHNIQUE
Anatomic | Graft Selection | Tunnel Placement
Critical ACL Reconstruction Technical Points
Femoral Tunnel
Anatomic placement in center of native footprint. Posterior to resident's ridge (anterior border of footprint). Transportal or outside-in technique. Avoid posterior blowout.
Tibial Tunnel
Center in native footprint. Posterior to anterior horn of lateral meniscus. Behind intersection of ACL stump and lateral meniscus. Too anterior = roof impingement in extension.
BTB Graft
Bone-to-bone healing in tunnels. Faster integration. Higher anterior knee pain and kneeling pain. Some evidence of lower re-rupture in young athletes.
Hamstring Graft
Soft tissue to bone healing (slower). Less anterior knee pain. Need minimum 8mm diameter for strength. May have hamstring weakness. Quadrupled graft common.
At a Glance
ACL reconstruction aims to restore knee stability through anatomic tunnel placement replicating native footprints, with tunnel position being the most critical technical factor. The femoral tunnel is placed posterior to the resident's ridge (anterior border of footprint) at approximately 10 o'clock (right knee) or 2 o'clock (left knee). The tibial tunnel center is positioned posterior to the anterior horn of the lateral meniscus—too anterior placement causes roof impingement in extension. Graft options include BTB (bone-to-bone healing, faster integration, more anterior knee pain), hamstring (less donor site morbidity, need ≥8mm diameter), quadriceps (increasing popularity), and allograft (revision/older patients). Grafts are tensioned at 15-20 degrees flexion. Return to sport rates are 85-90% with appropriate rehabilitation.
REARFemoral Tunnel Landmarks
Memory Hook:REAR = Behind Resident's ridge, at native footprint!
LMBTibial Tunnel Landmarks
Memory Hook:LMB = Lateral meniscus horn, Medial spine, Behind intersection!
BPKAGraft Selection - BTB vs Hamstring
Memory Hook:BPKA - BTB Pain, Kneeling issues, but remember 8mm minimum for All grafts!
Overview and Principles
ACL reconstruction aims to restore knee stability and allow return to pre-injury activity level. Modern technique emphasizes anatomic reconstruction replicating the native ACL footprints.
Anatomic Reconstruction
Anatomic single-bundle reconstruction places the graft in the center of the native ACL footprints. This contrasts with historical non-anatomic (isometric) techniques that placed the femoral tunnel more anterior and proximal.
Single vs Double Bundle
Most surgeons perform single-bundle reconstruction. Double-bundle (AM and PL bundles) aims to more closely replicate anatomy but has not shown clear superiority in outcomes.
Graft Selection
Bone-Patellar Tendon-Bone (BTB):
Advantages:
- Bone-to-bone healing in tunnels (faster, stronger integration)
- Some evidence of lower re-rupture in young athletes
- Historical "gold standard"
Disadvantages:
- Anterior knee pain (up to 20%)
- Kneeling pain
- Risk of patellar fracture, tendon rupture
- Fixed graft size
Use: First-time ACL reconstruction in young athletes, particularly if early return to high-level sport is priority.
Anatomy
Native ACL Anatomy
The anterior cruciate ligament originates from the posteromedial aspect of the lateral femoral condyle and inserts on the anterior tibial plateau, between the tibial spines.
Two Functional Bundles:
-
Anteromedial (AM) Bundle:
- More anterior and proximal femoral attachment
- Taut in flexion
- Primary restraint to anterior tibial translation
- Guides surgical technique in single-bundle reconstruction
-
Posterolateral (PL) Bundle:
- More posterior and distal femoral attachment
- Taut in extension
- Controls rotational stability
- Contributes to pivot shift phenomenon
Functional Significance: AM bundle controls anteroposterior stability; PL bundle controls rotational stability. Single-bundle reconstruction aims to replicate combined function.
Blood Supply and Innervation
Blood Supply: Middle genicular artery (branch of popliteal artery) provides majority of blood supply via synovial membrane. Poor intrinsic healing capacity explains need for reconstruction rather than repair.
Innervation: Posterior articular nerve (branch of tibial nerve). Contains mechanoreceptors (Ruffini endings, Pacinian corpuscles) important for proprioception.
Classification
ACL Injury Classification
ACL Injury Grades:
| Grade | Description | Clinical Features | Management |
|---|---|---|---|
| I (Sprain) | Mild stretch, intact fibers | Pain, minimal laxity, negative Lachman | Non-operative |
| II (Partial) | Partial tear, some fibers intact | Moderate laxity, soft endpoint | Variable - trial non-op vs reconstruction |
| III (Complete) | Complete rupture | Positive Lachman, pivot shift | Reconstruction in active patients |
Clinical Testing:
- Lachman test: Most sensitive (95%) - Grade 1 (3-5mm), Grade 2 (5-10mm), Grade 3 (greater than 10mm)
- Anterior drawer: Less sensitive than Lachman
- Pivot shift: Most specific for rotational instability
Clinical Assessment
History
Essential History Elements:
- Mechanism: Non-contact pivoting injury most common; contact injury may suggest multiligament injury
- Pop felt: 70% of patients describe audible/palpable pop
- Immediate swelling: Haemarthrosis develops within 4-6 hours (contrast with meniscal injury - delayed effusion)
- Inability to continue activity: Most cannot return to sport immediately
- Previous injuries: Prior ACL injury to same or contralateral knee
- Giving way episodes: Symptomatic instability since injury
Activity and Expectations:
- Sport type and level (pivoting vs linear sports)
- Occupational demands
- Expectation of return to sport
- Age and skeletal maturity
Examination
Key Clinical Tests:
| Test | Technique | Positive Finding | Sensitivity |
|---|---|---|---|
| Lachman | 20-30° flexion, anterior tibial translation | Soft endpoint, increased translation | 85-95% |
| Anterior Drawer | 90° flexion, anterior tibial translation | Increased translation | 40-50% |
| Pivot Shift | Valgus + internal rotation, flexion-extension | Clunk as tibia reduces | 35-95% |
| Lever Sign | Supine, fist under proximal tibia | Heel doesn't lift off bed | 80-90% |
Additional Assessment:
- ROM: Document any extension deficit
- Effusion: Large effusion suggests acute injury
- Collateral stability: MCL/LCL testing
- Meniscal signs: Joint line tenderness, McMurray's
- Neurovascular: Particularly if multiligament injury suspected
Investigations
Imaging Assessment
Standard Radiographs (AP, lateral, skyline):
Acute Findings:
- Usually normal
- Segond fracture: Avulsion of lateral tibial plateau rim - pathognomonic of ACL injury
- Tibial spine avulsion: Especially in adolescents
- Lateral capsular sign
Pre-operative Assessment:
- Joint space narrowing (osteoarthritis)
- Tunnel position from prior surgery (revision cases)
- Notch width: Narrow notch may increase impingement risk
- Limb alignment (varus/valgus)
Post-operative:
- Tunnel position assessment
- Hardware position
- Tunnel widening (follow-up)
Management
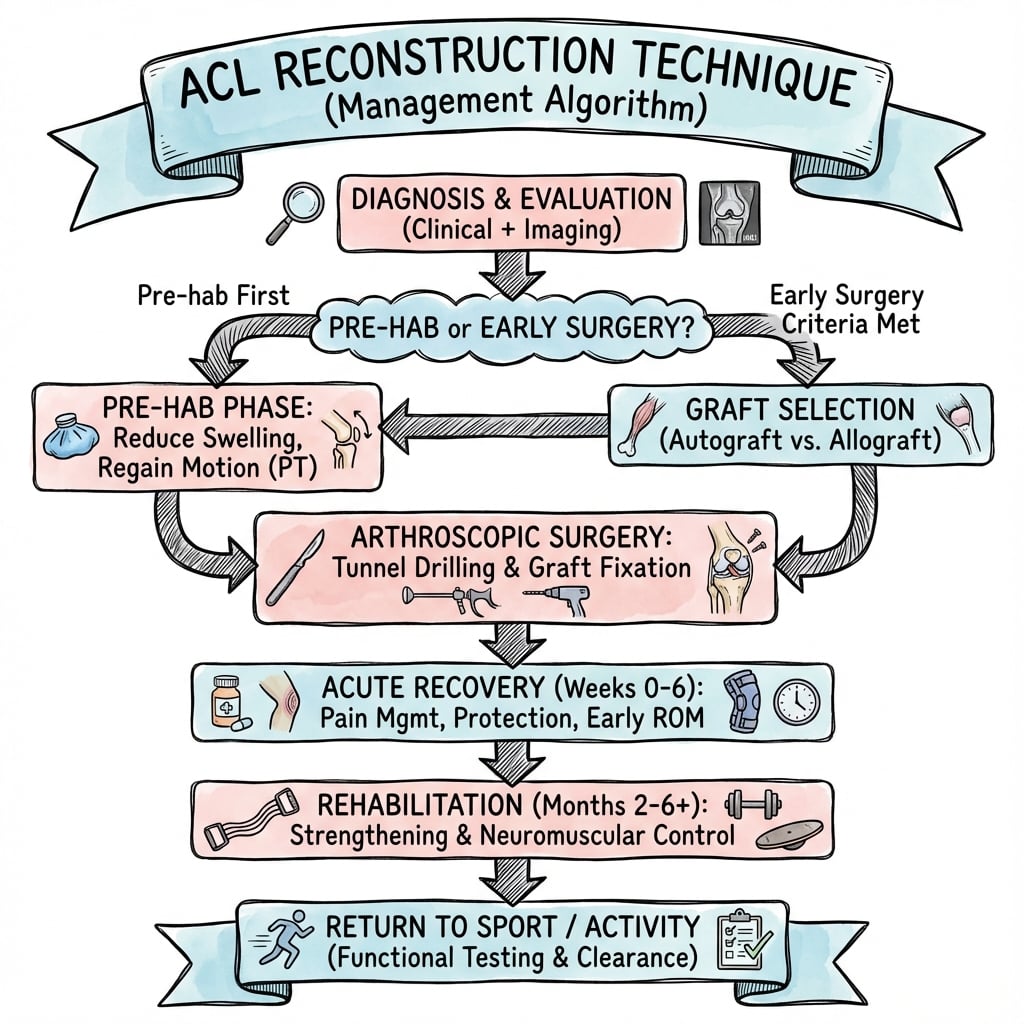
Treatment Algorithm
Indications for Non-operative Management:
- Low-demand patients
- Older, sedentary individuals
- No symptomatic instability
- Willing to modify activities
- Partial tears with minimal laxity
Non-operative Protocol:
-
Acute Phase (0-2 weeks):
- RICE protocol
- Protected weight-bearing
- Gentle ROM exercises
- Quadriceps activation
-
Rehabilitation Phase (2-12 weeks):
- Progressive strengthening
- Proprioceptive training
- Stationary cycling
- Aquatic therapy
-
Return to Activity:
- Functional brace for sport
- Avoid pivoting/cutting sports
- Activity modification
Failure of Non-operative Treatment: Symptomatic instability (recurrent giving way) despite rehabilitation indicates need for reconstruction.
Surgical Technique
Goal: Anatomic position in center of native femoral footprint.
Landmarks:
- Resident's ridge: Bony ridge marking anterior edge of footprint
- Posterior to resident's ridge
- Center of combined AM/PL footprint (single bundle)
Technique Options:
- Transportal: Drill through AM portal with knee hyperflexed. Better anatomic position.
- Transtibial: Drill through tibial tunnel. Historical technique, may limit anatomic positioning.
- Outside-in: Drill from lateral femoral cortex. Allows independent positioning.
Clock Position: 10 o'clock (right knee) or 2 o'clock (left knee) for single bundle. Avoid too vertical.
Complications
ACL Reconstruction Complications
Intraoperative Complications:
| Complication | Cause | Prevention/Management |
|---|---|---|
| Posterior blowout | Femoral tunnel too posterior | Careful guide placement, visualize posterior cortex |
| Graft damage | Improper handling, excessive tension | Avoid clamping, gentle passage |
| Neurovascular injury | Lateral femoral drill exit | Protect soft tissues, limit drill depth |
| Tunnel malalignment | Poor visualization, incorrect technique | Fluoroscopy, anatomic landmarks |
Early Post-operative (0-6 weeks):
- Haemarthrosis: Common, manage with aspiration if tense
- Infection: 0.5-1% incidence, aggressive treatment required
- DVT/PE: Thromboprophylaxis, early mobilization
- Nerve injury: Saphenous nerve (hamstring harvest), peroneal nerve (positioning)
Key Complication Prevention
- Tunnel position: Anatomic placement prevents impingement and improves outcomes
- Graft diameter: Minimum 8mm to reduce failure risk
- Timing: Avoid early surgery to prevent arthrofibrosis
- Rehabilitation: Protocol-based progression prevents re-rupture
Postoperative Care
Rehabilitation Protocol
Phase 1: Protection Phase (0-2 weeks)
Goals:
- Protect graft
- Control pain and swelling
- Restore full extension
- Achieve 90° flexion
Weight-Bearing:
- Partial weight-bearing with crutches
- Weight-bearing as tolerated by 2 weeks (graft dependent)
Exercises:
- Quadriceps setting (isometrics)
- Straight leg raises (when quad control achieved)
- Ankle pumps, heel slides
- Passive extension to 0° (critical)
- Patellar mobilization
Modalities:
- Ice, elevation
- Compression
- Gentle ROM exercises
Return to Sport Criteria
Modern protocols emphasize criteria-based rather than time-based return. Key metrics include:
- Quadriceps strength index greater than 90%
- Hop testing battery greater than 90%
- ACL-RSI psychological score greater than 70
- Completed sport-specific training without symptoms
Outcomes
ACL Reconstruction Outcomes
Overall Success Rates:
| Outcome Measure | Rate | Notes |
|---|---|---|
| Knee stability | 85-95% | Negative pivot shift |
| Return to sport | 65-85% | Same level as pre-injury |
| Patient satisfaction | 85-95% | IKDC, Lysholm scores |
| Graft survival | 85-90% at 10 years | Varies by graft type |
Functional Outcome Scores:
- IKDC subjective score: Improvement from 50 to 85+
- Lysholm score: Improvement to 85-90+
- Tegner activity scale: Often 1-2 levels below pre-injury
Long-term Considerations:
- 50-70% develop radiographic OA by 15-20 years
- Symptomatic OA less common
- Meniscal injury at time of ACL injury is major risk factor for OA
Evidence Base
Exam Viva Scenarios
Practice these scenarios to excel in your viva examination
Scenario 1: ACL Reconstruction Technique
"Describe your technique for ACL reconstruction in a 22-year-old footballer."
Scenario 2: Graft Selection Dilemma
"A 35-year-old tradesman who works on his knees needs ACL reconstruction. How do you counsel him about graft choice?"
Scenario 3: Post-operative Complication
"Six months post-ACL reconstruction, your patient has persistent loss of terminal extension. What is your approach?"
MCQ Practice Points
Q: What is the most common error in tibial tunnel placement?
A: Placing the tunnel too anterior. This causes roof impingement in extension, leading to graft failure, loss of extension, and anterior knee pain.
Q: What is the minimum recommended graft diameter for ACL reconstruction?
A: 8mm. MOON cohort data demonstrates that grafts less than 8mm in diameter have significantly higher failure rates. Always ensure adequate graft size.
Q: What is the resident's ridge?
A: A bony ridge on the lateral femoral wall that marks the anterior border of the native ACL femoral footprint. The femoral tunnel should be placed posterior to this landmark.
Q: What clock position is the femoral tunnel for a right knee?
A: 10 o'clock for right knee, 2 o'clock for left knee. This represents the center of the native ACL footprint and avoids the vertical (12 o'clock) position of older non-anatomic techniques.
Q: At what degree of knee flexion should ACL graft tensioning be performed?
A: 15-20 degrees of flexion. The knee should be cycled several times to eliminate creep before final fixation.
Australian Context
Australian ACL Practice
ACL Injury in Australia:
- Incidence: Approximately 17,000 ACL reconstructions performed annually
- Peak age group: 15-25 years
- Sex distribution: Males have higher absolute numbers; females have 2-3x higher rate in same sports
- High-risk sports: AFL, netball, soccer, rugby, skiing
Australian Football League (AFL):
- ACL injury rate: 0.8 per club per season
- Major cause of games missed
- Significant media and research attention
Netball:
- One of highest ACL injury rates in female sport
- Knee Injury Prevention Program (KIPP) widely promoted
AOSSM Guidelines
Australian surgeons follow international consensus on anatomic reconstruction with graft selection based on patient factors.
Prevention Programs
FIFA 11+, Netball Australia KNEE Program, and AFL-specific programs actively promoted in Australian sport.
ACL RECONSTRUCTION TECHNIQUE
High-Yield Exam Summary