Article summary
An evidence-backed guide to paediatric ACL injuries, including when to reconstruct early, how skeletal maturity changes technique choice, and why return-to-sport decisions cannot be based on time alone.
Educational content is reviewed for source visibility, editorial coherence, and correction readiness.
No individual clinician credential is claimed unless a named person is shown.
Verify before clinical use; this is not medical advice or a substitute for local guidance.
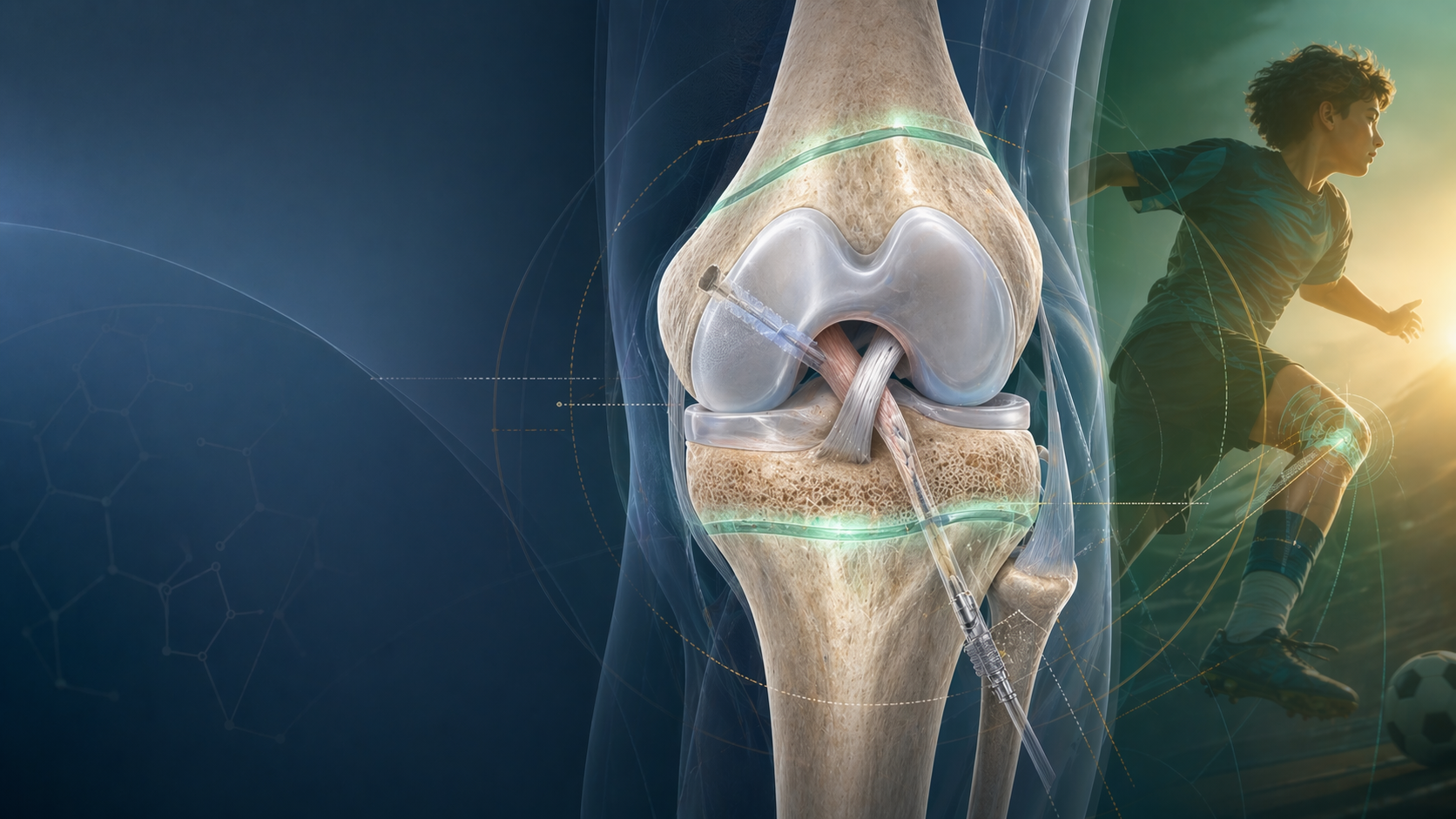
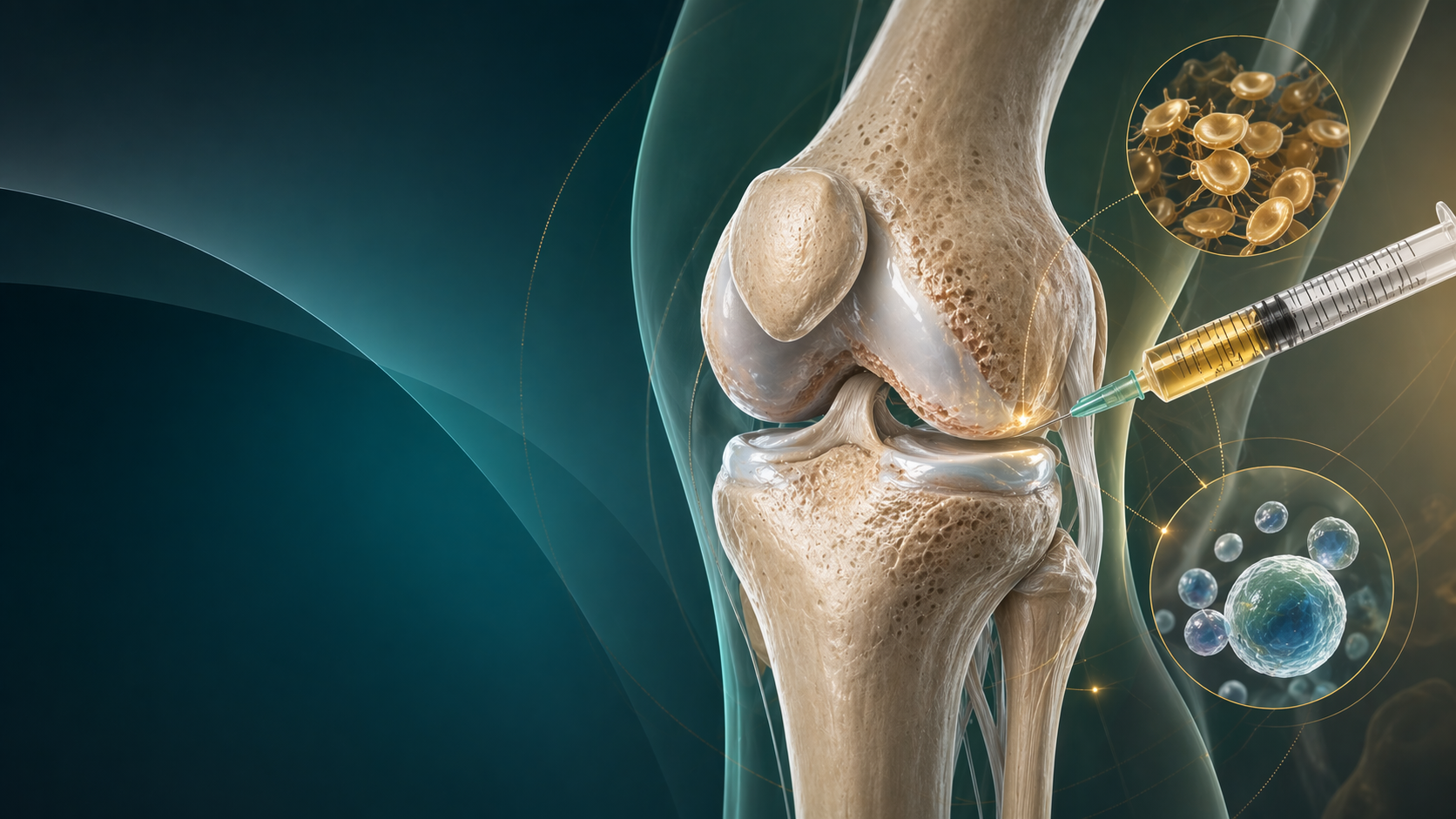
Paediatric ACL Tears in 2026: Physeal-Safe Reconstruction, Graft Choice, and Return to Sport
Paediatric ACL injuries are no longer unusual edge cases. Increased sports participation, year-round competition, and earlier specialisation mean trainees increasingly see unstable knees in children and adolescents who still have open physes. That changes the management discussion. In this group, the main question is not whether surgery carries growth-plate risk. It is how to balance that risk against the very real cost of recurrent instability, meniscal injury, and cartilage damage.
Fast Takeaways
- Unstable paediatric ACL tears managed with delay or repeated giving-way episodes risk secondary meniscal and chondral injury.
- Technique choice should follow skeletal maturity, not habit.
- Growth plate respect matters, but so does restoring stability in the right patient.
- Autograft-based reconstruction remains the backbone for most young athletic patients.
- Return-to-sport clearance must include strength, movement quality, confidence, and sport context, not just a date on the calendar.
Why This Matters in 2026
Modern paediatric ACL care is more sophisticated than the old surgery-versus-no-surgery debate. We now have a spectrum of physeal-sparing, physeal-respecting, and transphyseal options that can be matched to maturity and anatomy. That means the standard of care is increasingly about correct selection rather than blanket avoidance.
AAOS patient guidance reflects the direction of the field clearly: in children or adolescents with open growth plates, early reconstruction carries theoretical growth-plate risk, but delaying treatment can increase the risk of future meniscal and cartilage injury. That is exactly the balance trainees need to understand.
The Core Decision Points
1. Is the knee stable enough to live with?
Some partial tears and low-demand patients can be managed without immediate reconstruction, but the unstable child who keeps pivoting, subluxing, or returning to cutting sport is a different scenario. In that patient, recurrent instability can become the bigger harm.
The practical assessment includes:
- instability symptoms
- sport demands
- associated meniscal injury
- repairable meniscal pathology that benefits from stabilisation
- patient maturity and family reliability with rehabilitation
2. Match the reconstruction to skeletal maturity
The technique discussion should sound maturity-based:
- very immature patients may need physeal-sparing strategies
- patients approaching skeletal maturity can often be treated with physeal-respecting or carefully planned transphyseal reconstruction
- older adolescents with near-closed physes may be treated more like adult patients
The key is not memorising one preferred tunnel technique. It is showing that you understand why the physis matters and that the solution changes as remaining growth changes.
3. Choose the graft with the athlete in mind
Autograft remains the most defensible default in young athletic patients. The exact choice depends on age, sport, maturity, revision risk, and surgeon preference. The important principle for trainees is that graft choice should be an active decision, not an afterthought.
At a minimum, your counselling should address:
- donor site morbidity
- graft size and robustness
- graft failure risk
- previous surgery or associated injuries
4. Make return to sport a staged decision
The literature on paediatric return to sport remains messy, but one message is consistent: time alone is inadequate. A child can reach nine months post-op and still have poor strength symmetry, poor landing mechanics, low psychological readiness, or unrealistic sport exposure.
That is why good return-to-sport decisions should combine:
- objective strength testing
- hop or movement testing where appropriate
- patient-reported confidence
- sport demands
- the consequence of reinjury in that athlete
In paediatric ACL care, the safest plan is the one that protects the physis without leaving an unstable young athlete to damage the knee while waiting.
Common Pitfalls
Treating all open physes the same
There is a major difference between a child with years of growth remaining and an older adolescent nearing skeletal maturity. The surgical plan should reflect that.
Thinking only about the ACL
A paediatric ACL knee is often really a meniscus-protection problem as well. The ACL plan and the meniscus plan should be discussed together.
Making return to sport a date instead of a decision
If the child is weak, apprehensive, asymmetrical, or moving poorly, the calendar does not rescue the decision.
Assuming surgery alone solves reinjury risk
Rehabilitation quality, movement retraining, and sport-specific progression remain critical.
Exam and Practice Pearls
- In a viva, explicitly mention skeletal maturity before describing tunnels.
- Link the discussion to ACL injuries and tibial spine fractures if the stem is about children and knee instability.
- If asked whether early reconstruction is acceptable in children, say yes in selected unstable knees, provided the technique respects remaining growth.
- If asked about return to sport, say it is criteria-based and not time-only.
References
- ACL Injury: Does It Require Surgery? - AAOS OrthoInfo.
- Pediatric Anterior Cruciate Ligament Tears. 2024.
- Impact of Pediatric Knee Anatomy on ACL Reconstruction: Lessons Learned From Cadaveric Dissections. 2025.
- Reconsideration of Return-to-Sport Decision-Making After Pediatric ACL Injury: A Scoping Review. 2023.
Share this article
Useful for a journal club, study list, or teaching session.