Article summary
An evidence-backed guide to periprosthetic femur fractures around total hip arthroplasty, with a practical focus on stem stability, bone stock, Vancouver classification, and when to revise rather than plate.
Educational content is reviewed for source visibility, editorial coherence, and correction readiness.
No individual clinician credential is claimed unless a named person is shown.
Verify before clinical use; this is not medical advice or a substitute for local guidance.
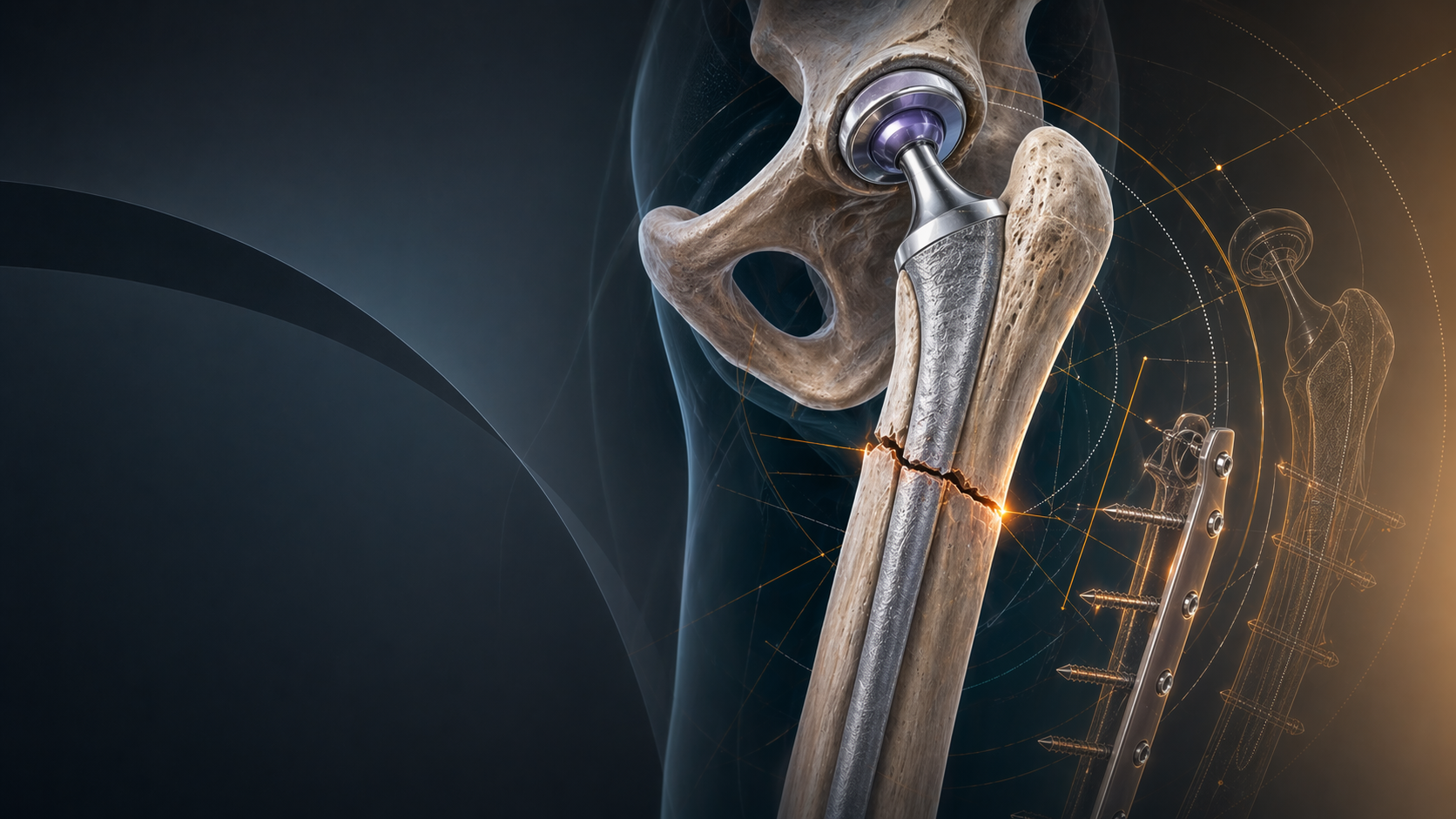
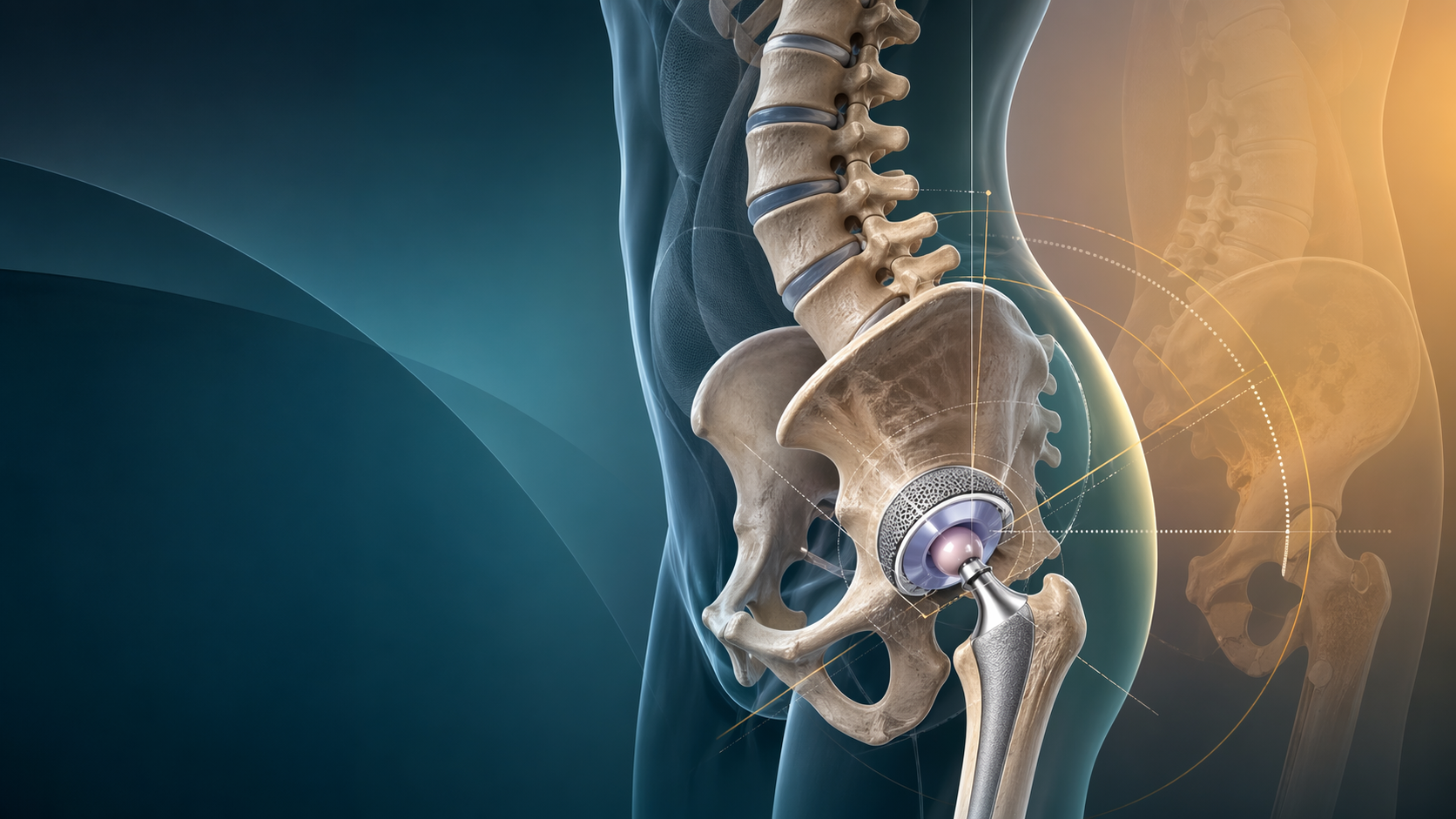
Periprosthetic Femur Fractures Around THA: A 2026 Vancouver-to-UCS Decision Guide
Periprosthetic femur fractures are one of the most demanding collisions between trauma and revision arthroplasty. They are increasingly common, they happen in frail patients and in younger active patients, and they punish poor classification. For trainees, the central task is not memorising letters. It is answering two questions correctly: is the stem loose, and is there enough bone stock to support the plan?
Fast Takeaways
- The Vancouver system is still clinically useful because it ties classification to treatment.
- The commonest major error is calling a B2 fracture a B1 fracture.
- If the stem is loose, fixation alone is rarely the right definitive answer.
- Intraoperative reassessment of stem stability is often decisive.
- These injuries often deserve management in centres comfortable with both revision arthroplasty and complex fixation.
Why This Matters in 2026
Total hip arthroplasty volume continues to rise, and with it the burden of periprosthetic fracture. The 2025 AOANJRR report reinforces the scale of revision work around conventional hip replacement and reminds us that fracture remains a meaningful failure mode in modern arthroplasty practice. That alone makes this an essential topic for on-call decision-making and fellowship exam preparation.
The 2025 review of the Vancouver classification “after 30 years” is a useful reminder that the system endures because it captures the three variables that actually matter:
- fracture location
- implant stability
- bone quality and bone stock
The newer Unified Classification System helps broaden the language across implant-related fractures, but day-to-day treatment planning still begins with Vancouver logic.
The Core Decision Points
1. Start with location, but do not stop there
Location gets you into the right neighbourhood:
- A fractures involve the trochanteric region
- B fractures are around or just below the stem
- C fractures are well distal to the stem
That is only the first step. The decisive branch inside type B is whether the stem is well fixed.
2. B1 versus B2 is the pivot point
This distinction changes everything:
- B1 means the stem is stable, so fixation is usually the main strategy.
- B2 means the stem is loose but proximal bone stock is still adequate, so revision femoral reconstruction is usually required.
- B3 means the stem is loose and the proximal femur is poor, so revision plus a bone-loss strategy is needed.
That is why good imaging, implant history, previous radiographs, and clinical suspicion matter so much. If the patient had pre-injury thigh pain, obvious subsidence, progressive radiolucency, or a stem pattern known for loosening, your threshold for calling the stem loose should fall.
3. Trust the operation more than a single radiograph
Pre-operative radiographs can strongly suggest stability or loosening, but they do not always settle the question. Many papers and algorithms emphasise that stem stability is sometimes definitively clarified only in theatre. A fracture that looks like a B1 on plain films can reveal a clearly unstable stem once exposed and tested.
For trainees, this is the practical lesson: plan with flexibility. If you are heading to theatre for what you think is a B1, the setup should still allow escalation if the stem proves loose.
4. Match the construct to the biology
Once stability is defined, treatment becomes more coherent:
- B1 fractures: fixation principles, bridging length, implant overlap, and biological preservation matter.
- B2 fractures: revision to a stem that bypasses the fracture and achieves fixation in healthier bone is usually the core move.
- B3 fractures: the problem is no longer “fix the fracture” alone. It becomes reconstruction of an elderly femur with poor remaining support.
This is why periprosthetic fracture work cannot be reduced to trauma plating alone. It sits squarely inside revision thinking.
B1 is usually a fixation problem. B2 is a stability problem. B3 is a stability-and-bone-loss problem.
Common Pitfalls
Accepting the first classification without challenging it
Classification should be a dynamic process that uses prior films, implant design, the fracture pattern, and intraoperative findings. If the plan depends on the stem being stable, you must actively prove that assumption.
Forgetting the patient’s pre-fracture story
Progressive thigh pain before the fall is a red flag. It suggests the fracture may have occurred on a background of stem loosening rather than around an otherwise healthy implant.
Treating every B2 patient as if they can tolerate any revision
The literature increasingly recognises the real-world tension between ideal biomechanics and frailty. That does not justify poor surgery, but it does mean operative strategy must respect physiology, mobility goals, and centre expertise.
Underestimating referral value
The best treatment can be transfer, not improvisation. An unstable stem in poor bone often needs revision-level equipment, implants, and personnel from the beginning.
Exam and Practice Pearls
- In a viva, say “I would classify it using Vancouver, but my definitive management depends on stem stability and bone stock.”
- Link your answer to periprosthetic hip fracture and arthroplasty imaging rather than speaking about plates in isolation.
- If asked about the UCS, explain that it extends periprosthetic fracture language, but the practical treatment logic around the femoral stem still mirrors Vancouver principles.
- If you are unsure between B1 and B2, say so, explain why, and describe how you will resolve the uncertainty.
References
- Treatment Algorithm of Periprosthetic Femoral Fractures. Orthopedic Reviews. 2022.
- Fractures of the Femur After Hip Joint Replacement: The Vancouver Classification After 30 Years. JBJS. 2025.
- Stem revision vs. internal fixation in Vancouver B2/B3 periprosthetic hip fractures: systematic review and meta-analysis. 2024.
- Effectiveness of open reduction internal fixation versus revision arthroplasty around Vancouver type B2 periprosthetic femoral fractures. BMC Musculoskeletal Disorders. 2025.
- AOANJRR 2025 Annual Report.
Related topics
Share this article
Useful for a journal club, study list, or teaching session.