Article summary
A practical 2026 guide to hip-spine syndrome for orthopaedic trainees. Learn how spinopelvic mobility changes functional cup position, why lumbar fusion matters, and how to reduce instability risk before THA.
Educational content is reviewed for source visibility, editorial coherence, and correction readiness.
No individual clinician credential is claimed unless a named person is shown.
Verify before clinical use; this is not medical advice or a substitute for local guidance.
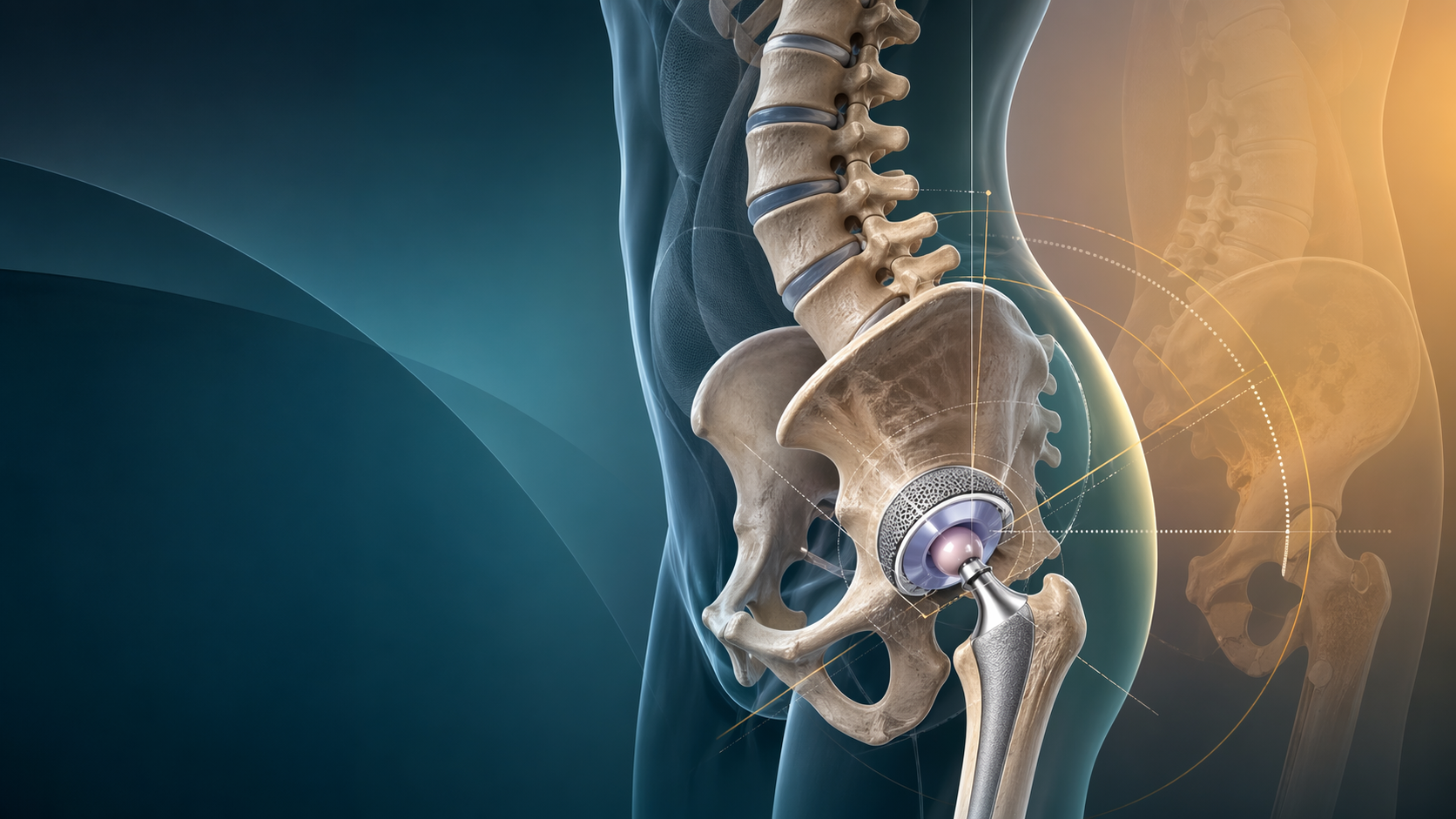
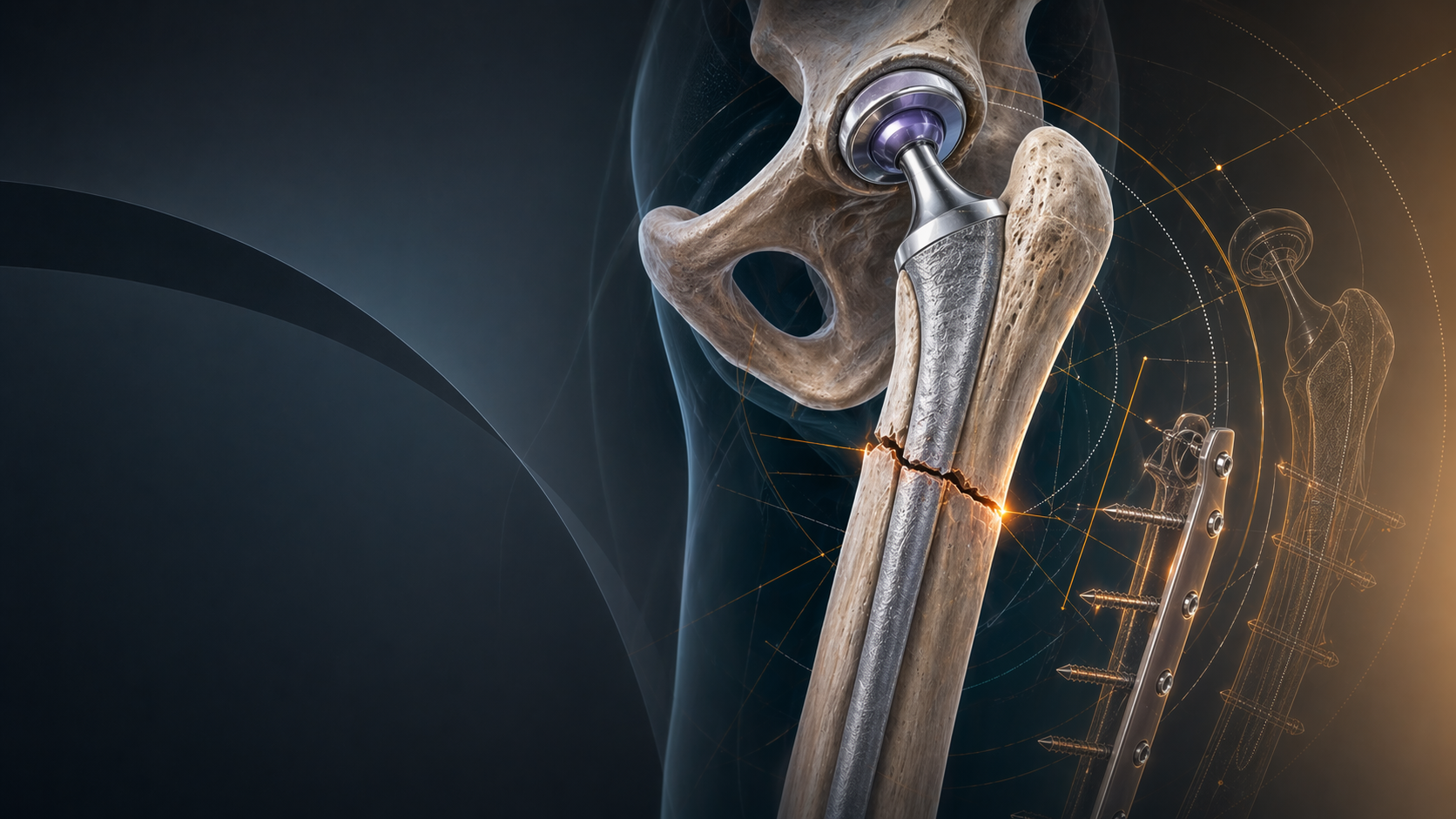
Hip-Spine Syndrome Before Total Hip Arthroplasty: Spinopelvic Mobility, Cup Position, and Instability Risk
The painful arthritic hip and the stiff degenerative lumbar spine often arrive together. That pairing matters because a technically well-positioned cup on a routine AP radiograph can still behave badly if the patient’s pelvis does not move normally between standing and sitting. For trainees, this is the heart of hip-spine syndrome in arthroplasty practice: component orientation is functional, not just static.
Fast Takeaways
- Spinopelvic stiffness changes how the acetabular component behaves during sitting and rising.
- Prior lumbar fusion, flatback deformity, and marked sagittal imbalance should trigger a higher-alert pre-operative workup.
- A single standing AP pelvis is not enough for every patient being considered for total hip arthroplasty.
- The key clinical question is not “where is the cup on X-ray?” but “how will this pelvis move after surgery?”
- Instability risk reduction starts before the incision with better phenotyping, not just with rescue choices in theatre.
Why This Matters in 2026
Hip arthroplasty remains one of the most successful operations in orthopaedics, but instability is still one of the commonest reasons for early failure and revision. At the same time, the arthroplasty population is older, more sagittally imbalanced, and more likely to have previous spinal surgery than it was a decade ago. That means the old habit of templating off a single AP pelvis and relying on a generic “safe zone” is increasingly incomplete.
Recent reviews emphasise that patients do not all move their pelvis in the same way. A normal pelvis posteriorly tilts when the patient sits, increasing functional acetabular anteversion. A stiff pelvis does that poorly, which can leave the hip relatively less anteverted in the seated position and more prone to posterior impingement and posterior instability. A hypermobile pelvis brings a different set of trade-offs. The practical consequence is simple: two patients can have the same cup position on paper and very different instability risk in real life.
The Core Decision Points
1. Identify the high-risk phenotype
Not every primary THA needs a complex spinopelvic workup. The patients who deserve extra attention are the ones with:
- previous lumbar fusion
- symptomatic lumbar degenerative disease
- obvious sagittal imbalance or flatback
- fixed flexion posture
- stiffness that does not match the apparent radiographic severity of hip arthritis
- prior instability, contralateral instability, or complex revision history
In these patients, a basic question helps: is the spine driving the pelvis, or is the hip driving the posture? If the lumbar spine cannot accommodate position change, the pelvis often cannot either.
2. Use imaging that answers a functional question
The most useful concept for trainees is that functional imaging should compare positions, not just document anatomy. Standing and sitting lateral views can help estimate how much the pelvis rotates between postures. That matters more than memorising one preferred measurement system.
The clinical aim is to decide whether the patient is:
- relatively stiff, with little postural pelvic change
- relatively normal, with expected posterior tilt on sitting
- hypermobile, with large positional change
This functional classification is more valuable than chasing perfect jargon. If you understand what the pelvis does when the patient sits down, you are already thinking correctly.
3. Plan the cup relative to movement, not in isolation
Cup orientation still matters, but its meaning changes when the pelvis behaves abnormally. In a stiff pelvis, the “same” cup can function as though it is less anteverted when seated. In a very mobile pelvis, the functional position may swing much more than expected. That is why the most important pre-operative planning step is integrating:
- spinal history
- standing posture
- sitting behaviour
- soft tissue tension
- implant strategy
This is also where implant choices such as larger heads or dual mobility constructs sometimes enter the conversation. They are not substitutes for thinking. They are adjuncts for a clearly identified risk pattern.
4. Respect the lumbar fusion patient
Lumbar fusion is not simply a background comorbidity. It changes the mechanics of the pelvis and can narrow the patient’s safe functional range. That does not mean every fused patient needs the same solution, but it does mean they deserve deliberate planning and a lower threshold for risk-mitigation strategies.
When the spine is stiff, the pelvis cannot reliably “save” a suboptimal cup position during posture change. That is why fused and sagittally imbalanced patients deserve more than routine templating.
Common Pitfalls
Treating hip-spine syndrome as a radiology buzzword
The diagnosis only becomes useful when it changes planning. If you write “hip-spine syndrome” in the notes but do not order functional views, examine posture, or modify strategy, the label has added nothing.
Over-relying on a single safe zone
The classic safe-zone idea helped standardise thinking, but it does not solve dynamic problems. Functional orientation can drift substantially with abnormal pelvic motion.
Ignoring the spine because the hip hurts more
Patients usually talk about the hip, limp, and loss of rotation. The lumbar spine can still be the key reason the arthroplasty is harder to plan safely.
Assuming lumbar fusion always means the same risk
The number of fused levels, residual sagittal balance, pelvic mobility, and symptoms all matter. A fused patient still needs individual assessment.
Exam and Practice Pearls
- In a viva, mention standing and sitting lateral imaging early. It shows you understand the dynamic problem.
- If asked why a “well-positioned” cup dislocated, explain the difference between static radiographic orientation and functional orientation.
- Link hip-spine thinking back to hip osteoarthritis and hip biomechanics, not just implant angles.
- If a patient has prior lumbar fusion plus high instability risk, say that you would plan the arthroplasty with that risk explicitly in mind rather than treating the fusion as incidental.
References
- Grammatopoulos G, Innmann M, Phan P, et al. Spinopelvic challenges in primary total hip arthroplasty. HIP International. 2023.
- Esposito CI, Miller TT, Kim HJ, et al. Implications of Spinopelvic Mobility on Total Hip Arthroplasty: Review of Current Literature. Journal of Orthopaedic Research. 2019.
- Pelvic version and kinematics in patients with total hip arthroplasty: a scoping review of current classification systems and recommendations based on spinal alignment. 2025.
- Creating Consensus in the Definition of Spinopelvic Mobility. 2023.
Related topics
Share this article
Useful for a journal club, study list, or teaching session.