Article summary
A 2026 guide to shoulder instability with glenoid bone loss, covering subcritical thresholds, CT planning, remplissage, and when Latarjet or bony augmentation should move to the front of the plan.
Educational content is reviewed for source visibility, editorial coherence, and correction readiness.
No individual clinician credential is claimed unless a named person is shown.
Verify before clinical use; this is not medical advice or a substitute for local guidance.
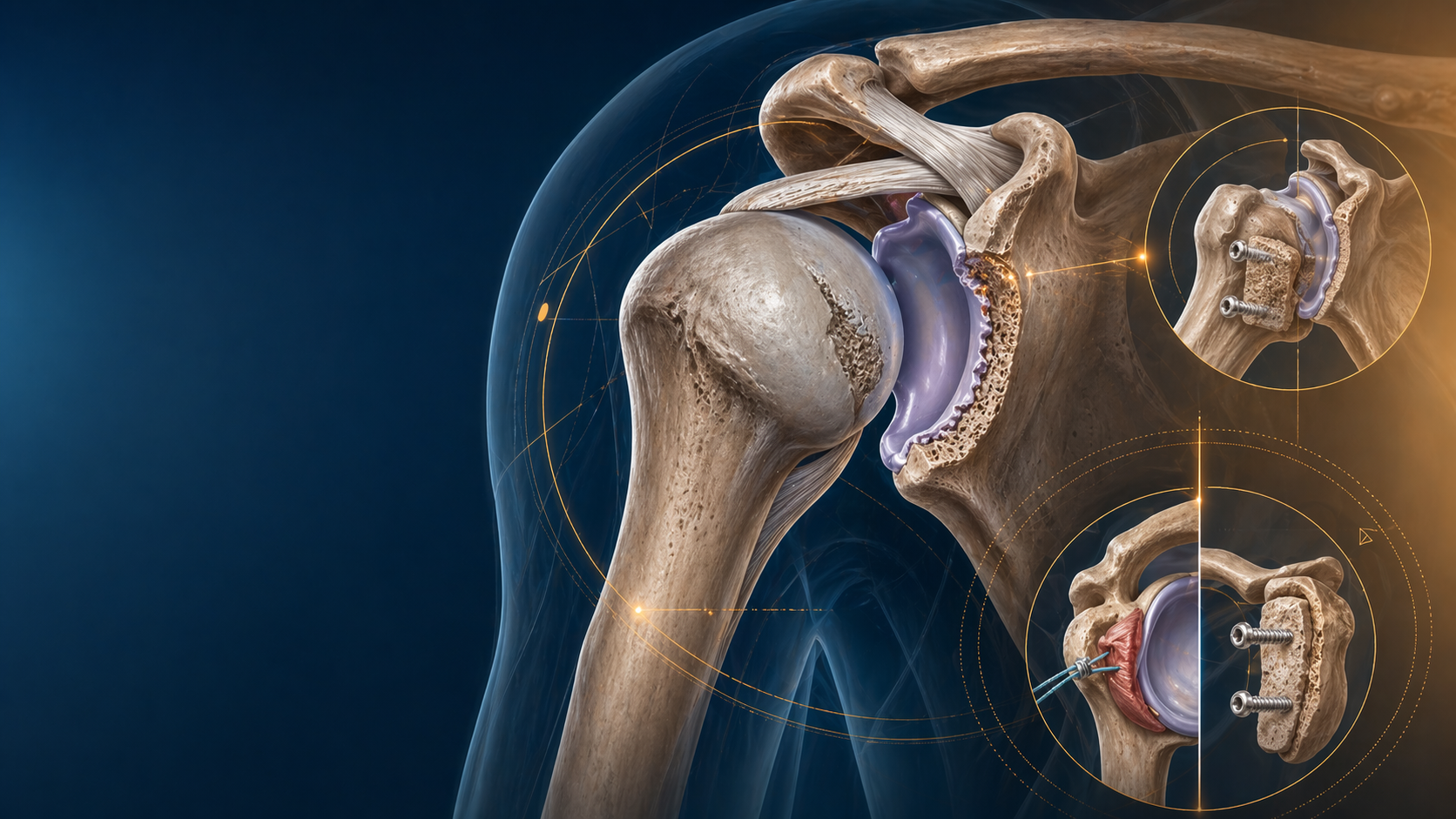
Shoulder Instability With Bone Loss: When Bankart Is Not Enough
The unstable shoulder with bone loss is where textbook soft-tissue thinking starts to break down. A trainee who only asks “labrum or no labrum?” will miss the real determinant of recurrence in many patients: the interaction between glenoid bone loss, humeral-sided lesions, and the demands being placed on the joint.
Fast Takeaways
- Bone loss changes the operation, not just the risk discussion.
- CT-based assessment of glenoid deficiency matters when instability is recurrent or high risk.
- “Subcritical” bone loss is clinically relevant even when the shoulder does not look catastrophically deficient.
- Remplissage has an important role in selected patients with engaging or high-risk Hill-Sachs lesions.
- Latarjet remains a powerful procedure, but it should be matched to the right problem rather than used as a reflex identity statement.
Why This Matters in 2026
The most useful shift in the modern literature is not a single magic number. It is the acceptance that clinically important bone loss begins earlier than many surgeons once thought. The old “critical” threshold of roughly 20% to 25% still matters for obvious deficiency, but more recent work has pushed attention toward subcritical loss because outcomes can deteriorate before the defect becomes dramatic on first glance.
That is why modern instability planning is less about a single threshold and more about risk architecture. Bone loss, Hill-Sachs behaviour, contact athlete profile, revision setting, tissue quality, and seizure or hyperlaxity context all change the answer.
The Core Decision Points
1. Measure the glenoid properly
If the patient has recurrent instability, especially after multiple events or failed previous repair, CT assessment becomes increasingly valuable. You need to know whether the glenoid is intact enough for a soft-tissue solution to succeed reliably.
This is also why the old habit of deciding purely from plain films and MRI can become risky in the high-demand shoulder.
2. Recognise that subcritical bone loss is not benign
Long-term follow-up data suggest that outcomes begin to worsen even below the classic catastrophic thresholds. The literature around 13% to 15% bone loss has pushed many surgeons to think more carefully about whether isolated Bankart repair is enough in high-risk patients.
This does not mean every patient with modest loss needs Latarjet. It means the defect can no longer be ignored simply because it looks “not that bad.”
3. Give remplissage its proper place
For many trainees, remplissage is introduced as an add-on. In reality, it is a major decision tool in the patient with anterior instability plus a risky humeral-sided lesion. In selected patients with subcritical glenoid loss, Bankart repair plus remplissage can produce outcomes that compare favourably with Latarjet in some series.
That makes it a procedure worth understanding well, not just name-dropping.
4. Know when the problem is bony enough to go bony
There are still patients in whom Latarjet or another bony augmentation procedure belongs near the front of the plan:
- significant glenoid loss
- failed prior soft-tissue repair
- high-risk contact athlete with repeated dislocation
- combined bipolar bone loss where a soft-tissue-only strategy looks underpowered
If the socket is too small for the ball you are trying to restrain, the answer is often not “repair the labrum tighter.” The answer may be to restore bony restraint.
Common Pitfalls
Pretending the threshold debate is settled
It is not. The smart move is to understand the direction of the evidence and the patient-specific modifiers, not to defend a single number like doctrine.
Ignoring the humeral side
Even a careful glenoid plan can fail if the Hill-Sachs lesion is clinically important and never enters the decision.
Using Latarjet as a personality trait
It is an excellent operation in the right patient. It is not a universal answer to every dislocator.
Underestimating revision context
The failed previous Bankart patient is not the same problem as the first-time instability patient with modest loss.
Exam and Practice Pearls
- Link the answer to anterior shoulder instability and glenoid bone loss rather than labral repair alone.
- If the case sounds recurrent and high demand, mention CT-based assessment early.
- Say that subcritical bone loss can still change the operation.
- Use remplissage and Latarjet as targeted tools, not slogans.
References
- Lau LCM, Chau WW, Ng R, et al. Reconsidering “Critical” Bone Loss in Shoulder Instability: 17-Year Follow-Up Study following Arthroscopic Bankart Repair. Advances in Orthopedics. 2024.
- Arthroscopic Bankart repair with remplissage yields similar outcomes to open Latarjet for primary and revision stabilization in the setting of subcritical glenoid bone loss. 2024.
- Multicentre randomised controlled trial comparing Bankart repair with remplissage and Latarjet procedure in shoulder instability with subcritical bone loss (STABLE): study protocol. 2024.
- Advancing surgical strategies for shoulder instability: Insights from AAOS 2025.
Share this article
Useful for a journal club, study list, or teaching session.