Radiological Signs in Bone Tumours
Aggressive vs Non-Aggressive Features & Pattern Recognition
Lodwick Classification for Bone Tumour Aggressiveness
Type IA: Geographic, well-defined sclerotic margin = benign (NOF, enchondroma, SBC)
Type IB: Geographic, well-defined NO sclerotic margin = low-grade malignant or aggressive benign
Type IC: Geographic, ill-defined margin = intermediate aggressiveness
Type II: Moth-eaten (multiple small lytic areas) = moderately aggressive malignancy
Type III: Permeative (cortical destruction, no defined margin) = highly aggressive malignancy
Key: The more well-defined and sclerotic the margin, the less aggressive the lesion
Critical Must-Knows
- Lodwick classification determines aggressiveness: geographic (I) = slow-growing, moth-eaten (II) = moderately aggressive, permeative (III) = highly aggressive.
- Codman triangle: periosteum lifted by tumour with reactive bone at the margin — does NOT represent tumour tissue itself (do not biopsy the Codman triangle).
- Matrix mineralisation pattern: chondroid (rings and arcs, stippled) vs osteoid (cloud-like, dense) — helps narrow the differential.
- Tumour location within the bone: epiphysis (GCT, chondroblastoma), metaphysis (osteosarcoma, chondrosarcoma), diaphysis (Ewing, lymphoma, fibrous dysplasia).
- MRI is essential for local staging: intramedullary extent, soft tissue mass, skip lesions, neurovascular involvement.
Examiner's Pearls
- "GCT: subarticular (epiphysis touching articular surface), eccentric, lytic, NO matrix mineralisation. Peak age 20-40. Knee region most common.
- "Osteosarcoma: metaphyseal, mixed lytic/scite, cloud-like osteoid matrix, Codman triangle, sunburst periosteal reaction. Peak age 10-25.
- "Ewing sarcoma: diaphyseal in children, permeative, lamellated (onion-skin) periosteal reaction, large soft tissue mass. Peak age 5-15.
- "Chondrosarcoma: medullary, rings and arcs calcification, endosteal scalloping more than two-thirds cortex, NO periosteal reaction (slow-growing).
- "Metastases are the MOST COMMON malignant bone tumour in adults over 40 (primary malignant tumours are rare at this age).
Exam Warning
Bone tumour radiological assessment is one of the highest-yield examination topics. You must be able to: classify aggressiveness using Lodwick criteria, identify periosteal reaction patterns, recognise matrix mineralisation, describe tumour location within bone, and outline the staging imaging pathway. Classic traps: not considering metastases as the most common malignant bone tumour in adults over 40, and confusing the Codman triangle with tumour tissue (it is reactive periosteum — do not biopsy it).
MAPLESBone Tumour Aggressiveness Assessment
Memory Hook:MAPLES: the systematic approach to bone tumour radiograph assessment — Margin, Age, Periosteal reaction, Location, Expansion, Struck-through matrix.
SCOLHPeriosteal Reaction Patterns
Memory Hook:SCOLH: periosteal reactions from most aggressive to least — Sunburst, Codman, Onion-skin, Lobulated, Hair-on-end.
EpiMeDiCommon Tumours by Location in Bone
Memory Hook:EpiMeDi: Epiphysis-Metaphysis-Diaphysis — know which tumours favour which location.
Overview
Radiological assessment of bone tumours requires a systematic approach that integrates multiple imaging features to narrow the differential diagnosis and determine aggressiveness. The key principles are: (1) assess the margin of the lesion (Lodwick classification), (2) evaluate the periosteal reaction pattern, (3) identify the matrix mineralisation, (4) note the location within the bone and the skeleton, and (5) consider the patient's age. These five features, assessed together, significantly narrow the differential diagnosis and guide further investigation.
The Lodwick Classification
The single most important radiographic feature is the MARGIN of the lesion, classified by Lodwick: Type IA — geographic destruction with a well-defined sclerotic rim. This is the classic appearance of benign lesions (non-ossifying fibroma, enchondroma, simple bone cyst). The sclerotic rim indicates the host bone is keeping pace with the lesion's growth. Type IB — geographic destruction with a well-defined margin but NO sclerotic rim. This suggests a low-grade malignancy or aggressive benign lesion (GCT, chondrosarcoma). Type IC — geographic with an ill-defined margin. Intermediate aggressiveness. Type II — moth-eaten pattern (multiple small lytic areas without defined margins). Moderately aggressive malignancy. Type III — permeative pattern (cortical destruction without any defined lesion margin). Highly aggressive — Ewing sarcoma, osteosarcoma, lymphoma, metastases.
Staging Imaging Protocol
When a bone tumour is suspected: (1) Plain radiograph: ALWAYS the first investigation. Provides the most diagnostic information for pattern recognition. (2) MRI of the ENTIRE involved bone (including the joint above and below): shows intramedullary extent, soft tissue mass size, skip lesions, and neurovascular relationship. Essential for surgical planning. (3) CT chest: MUST be performed for pulmonary metastasis staging (the lungs are the most common site of metastasis for primary bone tumours). (4) Bone scan or PET-CT: for skeletal staging (detecting other skeletal lesions). (5) CT-guided biopsy: for histological diagnosis. CRITICAL: the biopsy tract must be planned with the surgeon who will perform the definitive surgery — a poorly placed biopsy contaminates tissue planes and may compromise limb salvage surgery.
Clinical Imaging
Imaging Gallery
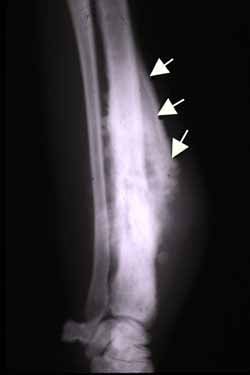
Systematic Approach
Bone Tumour Pattern Recognition
Classic Bone Tumour Patterns by Diagnosis
| Tumour | Radiographic Features | Key Distinguishing Feature |
|---|---|---|
| Osteosarcoma | Metaphyseal, mixed lytic/sclerotic, cloud-like osteoid matrix, Codman triangle, sunburst periosteal reaction | Cloud-like mineralisation + aggressive periosteal reaction. Peak age 10-25. Around knee (60%) |
| Ewing sarcoma | Diaphyseal (in children), permeative, lamellated (onion-skin) periosteal reaction, LARGE soft tissue mass | Permeative destruction + large soft tissue mass disproportionate to bone lesion. Peak age 5-15 |
| Chondrosarcoma | Medullary, rings and arcs calcification, endosteal scalloping more than two-thirds cortex, NO periosteal reaction | Rings and arcs matrix + endosteal scalloping. Peak age 40-60. Slow-growing, rarely metastasises |
| Giant cell tumour | Subarticular (epiphyseal), eccentric, well-defined lytic, NO matrix, NO sclerotic rim (Lodwick IB) | Epiphyseal location touching articular surface in CLOSED physis. Peak age 20-40. Knee region |
| Simple bone cyst (SBC) | Central metaphyseal, well-defined lytic, thin sclerotic rim, fallen fragment sign (pathological fracture) | Central location. Fallen fragment sign = fragment falls to dependent portion of cyst. Age 5-15 |
| Non-ossifying fibroma (NOF) | Eccentric metaphyseal, well-defined scalloped sclerotic rim, cortically based (bubbly) | Most common incidental bone lesion. Lodwick IA. Cortical thinning without breach. Age 10-20. No treatment |
| Enchondroma | Central, well-defined lytic with rings and arcs calcification, NO periosteal reaction, hands most common | Chondroid matrix (rings and arcs) in a small bone of the hand = virtually diagnostic. No treatment unless symptomatic |
| Metastases | Over 40 years. Lytic (most), blastic (prostate, breast), or mixed. Pedicle destruction on spine (winking owl) | MOST COMMON malignant bone tumour in adults over 40. Usually multiple. Common primary: lung, breast, kidney, thyroid, prostate |
Evidence Base
MRI for Local Tumour Staging
- MRI accurately assessed intramedullary tumour extent in 97% of cases (vs 80% for CT).
- MRI detected skip lesions (separate foci of tumour within the same bone) in 5% of cases that were missed by CT and radiographs.
- MRI was superior for assessing soft tissue mass extent and neurovascular involvement.
Lodwick Classification and Tumour Behaviour
- Lodwick IA lesions (geographic, sclerotic margin) were benign in 95% of cases.
- Lodwick II-III lesions (moth-eaten, permeative) were malignant in more than 90%.
- The classification had high inter-observer reliability and predicted behaviour accurately.
Staging imaging evidence guides the assessment of bone tumours.
Australian Context
In Australia, bone tumour management follows the multidisciplinary team (MDT) approach through specialised sarcoma units located in major metropolitan hospitals. The National Bone and Soft Tissue Tumour Registry and the Australian Sarcoma Group coordinate care and research. RANZCR guidelines mandate whole-bone MRI and CT chest as standard staging investigations before biopsy.
Australian orthopaedic guidelines emphasise referral to a specialist sarcoma centre BEFORE biopsy, consistent with international evidence that referral centre biopsy significantly reduces amputation rates and treatment complications. CT-guided core biopsy is the preferred technique at most Australian sarcoma centres.
Exam Viva Scenarios
Practice these scenarios to excel in your viva examination
"An examiner shows you a radiograph of the distal femur in a 16-year-old boy with knee pain. The radiograph shows a mixed lytic and sclerotic lesion in the metaphysis with cloud-like mineralisation, cortical destruction, and a Codman triangle."
"A 30-year-old woman presents with a lytic lesion in the proximal tibial epiphysis that extends to the articular surface. There is no matrix mineralisation."
"An examiner asks you to describe the systematic approach to assessing a bone tumour on a plain radiograph."
Bone Tumour Radiological Signs — Exam Day Reference
High-Yield Exam Summary
MAPLES Systematic Assessment
- •Margin (Lodwick): IA (sclerotic = benign), IB-IC (no sclerosis), II (moth-eaten), III (permeative)
- •Age: under 5 (LCH, neuroblastoma), 5-25 (Ewing, OS), 20-40 (GCT), over 40 (METASTASES)
- •Periosteal: solid (benign), onion-skin (Ewing), sunburst (OS), Codman triangle (aggressive)
- •Location: epi (GCT), meta (OS, SBC), dia (Ewing). Position: central vs eccentric
- •Matrix: cloud-like = osteoid (OS), rings/arcs = chondroid (enchondroma/CS), none = GCT/mets
Classic Tumour Patterns
- •Osteosarcoma: metaphyseal, cloud-like matrix, sunburst, Codman, age 10-25, around knee
- •Ewing: diaphyseal, permeative, onion-skin, LARGE soft tissue mass, age 5-15
- •GCT: subarticular epiphyseal, eccentric, lytic, NO matrix, Lodwick IB, age 20-40
- •Enchondroma: central, rings/arcs, hands. Chondrosarcoma: same matrix but endosteal scalloping
- •Metastases: most common malignant tumour over 40. Lytic (most), blastic (prostate/breast)
Staging Protocol
- •MRI: entire involved bone (skip lesions), soft tissue extent, NV bundle
- •CT chest: ESSENTIAL (pulmonary mets = most common site for primary bone tumours)
- •Bone scan/PET-CT: skeletal staging (other bone lesions)
- •Biopsy: REFER to sarcoma centre FIRST. Tract must be excisable en bloc
- •Codman triangle = reactive periosteum — do NOT biopsy it