Weight-Bearing CT: Principles & Applications
Cone-Beam CT Under Physiological Load
Highest-Yield WBCT Use Cases
Critical Must-Knows
- WBCT is primarily a bone and alignment tool, not a soft-tissue replacement for MRI.
- Use WBCT when symptoms are load-dependent: syndesmosis, hindfoot valgus/varus, Lisfranc instability, ankle malreduction.
- The main advantage over conventional CT is physiologic loading, not simply another cross-sectional scan.
- Contralateral comparison is high yield for subtle syndesmotic or midfoot instability.
- If the patient cannot safely weight-bear, standard CT or MRI is usually the correct alternative.
Examiner's Pearls
- "Syndesmotic instability may look reduced on supine CT but widen in loaded position.
- "WBCT improves hindfoot moment-arm and 3D alignment assessment compared with projection-dependent radiographs.
- "WBCT is strongest for foot and ankle bone questions; MRI remains better for tendon, ligament, cartilage, and marrow oedema questions.
- "Do not order WBCT just because it is newer; order it when loading is likely to change the answer.
Do Not Use WBCT as a Default CT Substitute
WBCT adds value only when the clinical question is load-dependent. If the patient cannot stand, or if the question is tendon, ligament, marrow, tumour, or infection extent, conventional CT or MRI is usually more appropriate.
LOAD Indications
Memory Hook:Order WBCT when loading reveals the pathology.
STAND Review Sequence
Memory Hook:STAND keeps the report focused on what changes under load.
Overview
WBCT is usually performed on a cone-beam platform with the patient standing, semi-standing, or otherwise positioned to load the limb during acquisition. The key orthopaedic advantage is that loaded alignment, joint congruity, and subtle instability can be measured directly instead of inferred from projectional radiographs or from unloaded CT.
The practical scope remains foot-and-ankle dominant. The literature is strongest for syndesmosis assessment, adult-acquired flatfoot, cavovarus deformity, hallux valgus planning, ankle osteoarthritis, and post-operative reduction analysis. Outside those indications, WBCT is still emerging and should not be treated as a universal replacement for conventional CT.
Clinical Imaging
Imaging Gallery
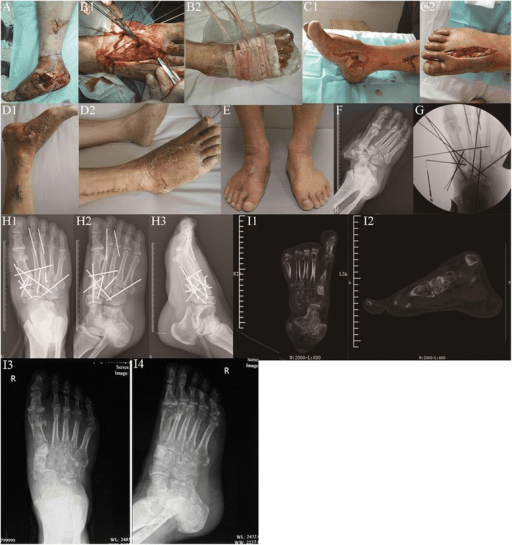
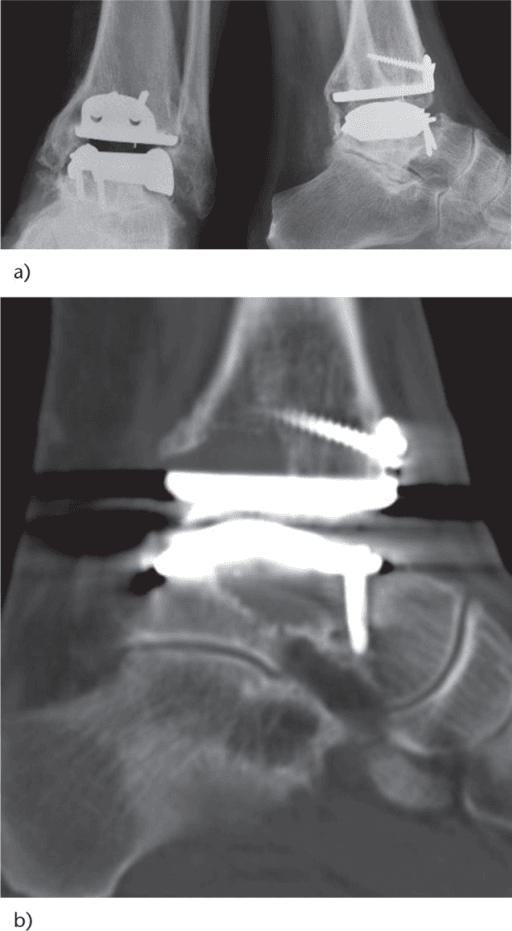
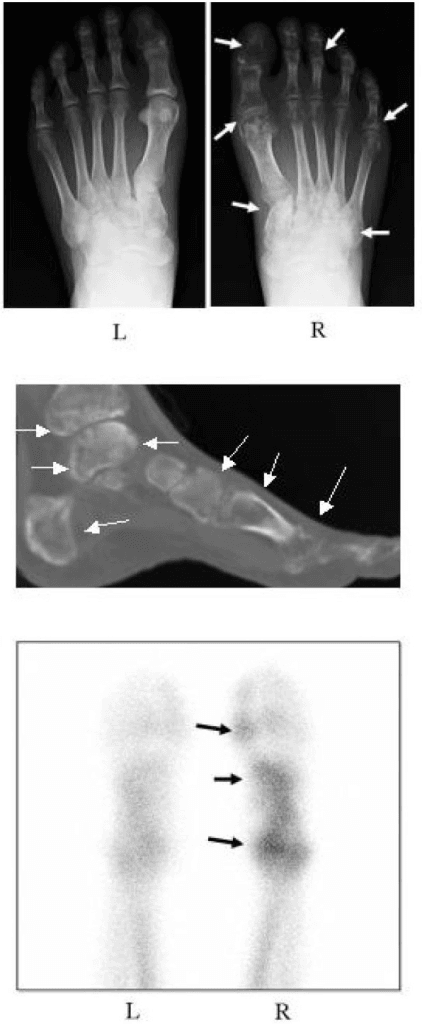
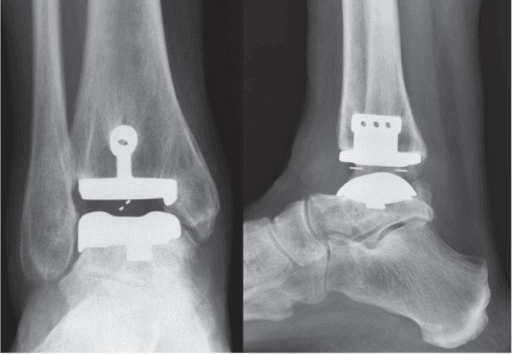
Systematic Approach
Systematic WBCT Review
| Step | Question | Why it matters |
|---|---|---|
| 1. Global alignment | Is there valgus, varus, arch collapse, or rotational asymmetry? | Defines the deformity plane before drilling into joints |
| 2. Joint congruity | Do the ankle, subtalar, talonavicular, and TMT joints remain congruent under load? | Loaded incongruity can explain symptoms despite normal supine imaging |
| 3. Syndesmosis or midfoot interval | Is there diastasis or malreduction relative to the contralateral side? | High-yield indication for WBCT |
| 4. Bone response | Are there cysts, osteophytes, subchondral changes, or occult fracture lines? | Adds surgical-planning detail |
| 5. Bilateral comparison | Does the symptomatic side deviate meaningfully from the opposite side? | Reduces over-calling subtle anatomic variation |
Reporting Principle
Clinical Applications
Why WBCT Helps the Syndesmosis
| Problem | What WBCT adds | Clinical use |
|---|---|---|
| Subtle instability | Shows widening or fibular malposition under load | Diagnose occult instability |
| Post-fixation assessment | Quantifies residual diastasis or rotational malreduction | Check reduction quality |
| Equivocal radiographs | Provides bilateral cross-sectional comparison | Resolve borderline cases |
High-Yield Point
Limitations
Limitations of WBCT
| Limitation | Why it matters | Preferred alternative |
|---|---|---|
| Cannot stand safely | The test loses its core advantage | Conventional CT or MRI |
| Soft tissue question | Tendon, ligament, cartilage, and marrow detail are limited | MRI |
| Restricted access | Equipment remains concentrated in specialist centres | Conventional imaging pathway |
| Motion artefact | Standing acquisition can degrade images in painful patients | Shorter protocols or alternative imaging |
Evidence Base
Systematic Review of WBCT in Foot and Ankle Surgery
- WBCT was most consistently useful for hindfoot alignment, syndesmotic assessment, and deformity analysis in the available literature.
- Loaded imaging frequently demonstrated greater deformity or instability than non-weight-bearing studies.
- The review identified the strongest clinical adoption in foot and ankle surgery rather than across all orthopaedic subspecialties.
Reproducibility of WBCT Measurements
- WBCT produced reproducible 3D measurements of foot and hindfoot position in clinical use.
- The technique improved appreciation of loaded alignment beyond what is visible on supine CT.
- The authors highlighted value for multiplanar deformity assessment and pre-operative planning.
Loaded Alignment Compared with Alternative Weight-Bearing Assessment
- WBCT provided weight-bearing alignment information while preserving superior osseous detail compared with lower-detail alignment studies.
- Cross-sectional reformats improved understanding of hindfoot and ankle position in complex deformity.
- The study supported WBCT as a combined alignment-and-planning test for selected cases.
Exam Viva Scenarios
Practice these scenarios to excel in your viva examination
"A patient has persistent syndesmotic tenderness despite normal radiographs and non-weight-bearing CT."
"You are planning surgery for adult-acquired flatfoot deformity."
"A patient with possible Lisfranc injury has equivocal radiographs and ongoing midfoot pain."
Weight-Bearing CT Quick Reference
High-Yield Exam Summary
Best Indications
- •Syndesmotic instability or malreduction
- •Hindfoot valgus or cavovarus assessment
- •Equivocal Lisfranc instability
- •Complex post-operative alignment review
Systematic Review
- •Assess global stance alignment first
- •Check joint congruity under load
- •Quantify interval widening or malrotation
- •Compare with contralateral side when possible
Strengths
- •3D loaded osseous assessment
- •Better deformity quantification than projectional views
- •Useful surgical-planning detail
- •Particularly strong in foot and ankle practice
Limitations
- •Needs safe weight-bearing
- •Poor soft-tissue characterisation compared with MRI
- •Restricted availability
- •Not a universal replacement for conventional CT