Article summary
A practical evidence-based guide to distal radius fractures in older adults, covering when casting is enough, when volar plating helps, and why functional age matters more than chasing perfect radiographs.
Educational content is reviewed for source visibility, editorial coherence, and correction readiness.
No individual clinician credential is claimed unless a named person is shown.
Verify before clinical use; this is not medical advice or a substitute for local guidance.
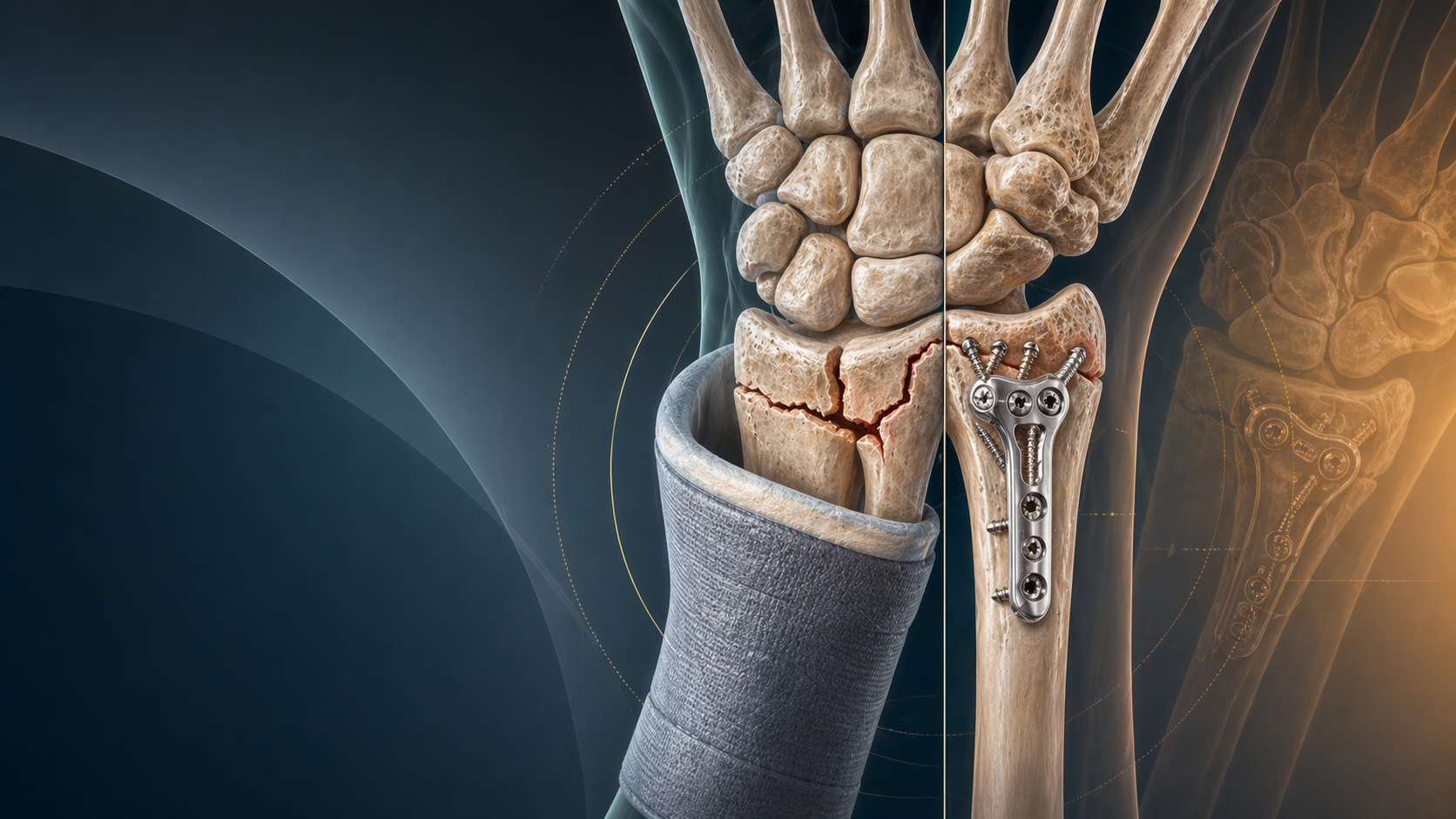
Distal Radius Fractures in Older Adults: When Surgery Helps and When It Does Not
Distal radius fractures in older adults are a perfect example of how orthopaedics can drift away from the outcomes that matter. The radiographs tempt us to chase reduction. The patient often wants independence, pain control, and a usable hand. Those goals overlap, but they are not identical. The best recent evidence keeps returning to the same point: better-looking X-rays do not automatically translate into better long-term patient-reported outcomes in older adults.
Fast Takeaways
- For many patients aged 65 years and older, surgery does not clearly improve long-term patient-reported outcomes compared with nonoperative care.
- Volar locking plates may improve early recovery, but that short-term gain is not the same as better one-year function.
- Functional demand, cognition, independence, and comorbidity often matter more than chronological age alone.
- Some older adults still benefit from surgery, especially if they are active and high-demand.
- Every low-energy distal radius fracture in an older patient should trigger a bone health conversation.
Why This Matters in 2026
The AAOS and ASSH distal radius guideline remains one of the clearest evidence summaries in trauma. Its message is striking: in geriatric patients, operative treatment does not lead to improved long-term patient-reported outcomes compared with nonoperative treatment. Newer data, including the DART trial, continue to reinforce the core idea that casting often performs better than many surgeons intuitively expect.
That does not mean surgery is never useful. It means the indication should be functional and patient-specific, not a reflex response to displacement alone.
The Core Decision Points
1. Decide whether this is truly a low-demand wrist
Not every patient older than 65 is low demand. A robust, independent, highly active older adult may value faster return of wrist function and may tolerate surgery well. A frailer patient with major comorbidity, limited ambulation, or low functional demand may gain little from plating a fracture that can be managed acceptably in a cast or splint.
This is why the smartest question is often: what does this patient need the wrist to do in the next three months, and what are they likely to care about in one year?
2. Know what surgery is buying
In many older adults, volar plating buys:
- better radiographic alignment
- earlier recovery of some function
- the possibility of quicker independence with hand use
What it may not reliably buy is clearly better long-term patient-reported function. That distinction is crucial. If the patient values early function enough, surgery may still be reasonable. But the conversation should be honest.
3. Nonoperative care is active treatment, not neglect
A well-moulded cast or splint, appropriate follow-up, swelling control, and early finger motion are all part of good care. Nonoperative treatment should not be framed as “doing nothing.” For many older adults, it is the evidence-based default.
4. Use fracture pattern and red flags sensibly
There are still clear reasons to escalate:
- open injury
- neurovascular compromise
- irreducible deformity
- fracture-dislocation pattern
- associated carpal instability
- patient-specific functional reasons that make early restoration especially important
The mistake is not operating on these patients. The mistake is treating every displaced fracture in an older adult as though perfect alignment is the only meaningful endpoint.
In older adults, ask whether surgery changes the patient’s lived outcome in a meaningful way. If the likely gain is mostly radiographic, slow down and reconsider.
Common Pitfalls
Using age alone as the indication
Chronological age is a poor substitute for functional age. Some older adults deserve more aggressive treatment, but that should be because of who they are and how they live, not because a number triggered a habit.
Under-counselling about what plating actually changes
If you do not explain the difference between early improvement and long-term outcome, patients can leave with unrealistic expectations.
Missing the osteoporosis opportunity
A low-energy distal radius fracture may be the first visible fragility fracture. If the wrist is treated but the bone health story is ignored, the system has missed a chance to prevent a hip or vertebral fracture later.
Over-reading a good reduction
A beautifully reduced fracture in theatre is not a patient-reported outcome. Keep the endpoint honest.
Exam and Practice Pearls
- Quote the broad AAOS/ASSH message: older adults generally do not gain better long-term patient-reported outcomes from routine operative fixation.
- Mention that volar locking plates can improve short-term function, which is where the shared decision-making nuance lies.
- Link the case to osteoporosis if the injury was low energy.
- If asked who among older adults should still be considered for surgery, discuss physiologic age, independence, and irreducible or unstable patterns.
References
- Management of Distal Radius Fractures Evidence-Based Clinical Practice Guideline. AAOS and ASSH.
- Cast Versus Surgery for Displaced Intra-Articular Distal Radius Fractures in the Elderly (DART Study). 2025.
- Comparison of Distal Radius Fracture Outcomes in Older Adults Stratified by Chronologic vs Physiologic Age Managed With Casting vs Surgery. 2023.
- Nonsurgical Management of Distal Radius Fractures in the Elderly: Approaches, Risks and Limitations. 2022.
Share this article
Useful for a journal club, study list, or teaching session.